Recently, a new offshoot of the Delta variant has been gaining ground in the U.K. It’s called AY.4.2, and it appears to be slightly more transmissible than Delta itself. While experts say this variant doesn’t differ enough from Delta to pose a serious concern, I think it’s worth exploring what we know about it so far—and what this means for the future of coronavirus mutation.
How was AY.4.2 identified?
The U.K. national health agency first found AY.4.2 in July 2021, and has watched it slowly spread through the country since then. The agency formally designated this variant as a Variant Under Investigation (VUI) on October 22; at this point, about 15,000 cases had been identified across the country.
It’s worth noting here that the U.K.’s genomic surveillance system is incredibly comprehensive—considered to be the best in the world. The country sequences over 20,000 coronavirus samples a week; it’s consistently sequenced a large share of its COVID-19 cases since the beginning of 2021. And, since the country’s public health system integrates COVID-19 testing records with hospitalization records, primary care records, and other data, U.K. researchers are able to analyze other aspects of a variant’s performance, such as its ability to cause breakthrough cases or more severe disease.
As STAT News’ Andrew Joseph explains in a recent story about this variant:
It’s perhaps not a surprise that the U.K. noticed AY.4.2 so quickly. The country has an incredible sequencing system in place to monitor genetic changes in the virus, and researchers there have been among the global leaders in characterizing different mutations and forms of the virus. It’s possible that other Delta sublineages have similar growth rates to AY.4.2, but they’re in parts of the world where it will take longer for scientists to detect.
How does AY.4.2 differ from OG Delta?
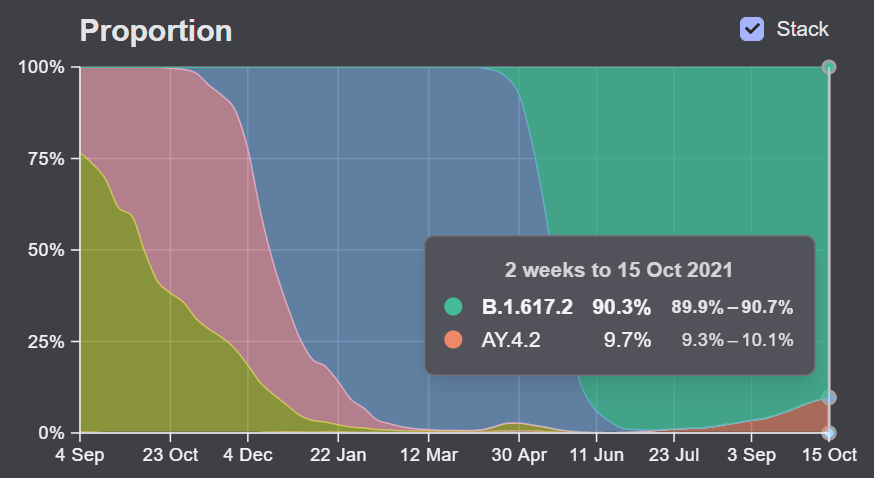
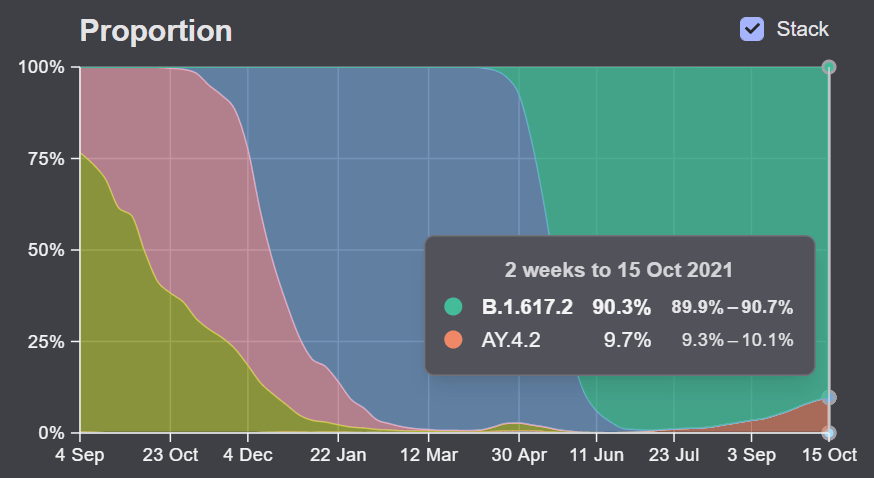
AY.4.2 is transmissible enough that it is slowly pushing out the original Delta in some parts of the U.K. In late June, it comprised 0.1% of new U.K. COVID-19 cases; in late August, it was at 3.5%; and now it’s at 11.3%, as of the most recent data (the week ending October 24).
“It’s a slow burner,” wrote U.K. epidemiologist Meaghan Kill in a Twitter thread last week. “But Delta is already *so* transmissible, it’s notable that AY.4.2 is increasing in that context.”
Kill and other scientists estimate that AY.4.2 is between 10% and 15% more transmissible than Delta. That’s a small enough difference that scientists are not panicking about this variant, in the same way that epidemiologists sounded the alarm when Delta itself was first identified in India earlier in 2021. (For context: Delta is 60% to 80% more transmissible than the Alpha variant.)
Still, AY.4.2 is worth watching as a signal of Delta’s continued ability to mutate and spread more readily. As Joseph points out in his STAT article, some experts hypothesized that Delta might be so contagious, the coronavirus basically could not mutate further in that direction. AY.4.2 suggests that we haven’t hit that upper limit yet.
Is AY.4.2 more likely to cause breakthrough cases?
This is one piece of good news that came out in the U.K. health agency’s most recent variant report, released this past Friday: AY.4.2 is not more likely to cause a breakthrough case than the original Delta variant. (Not thus far, anyway.) This is true for both symptomatic and asymptomatic infections, as well as different ages and vaccine types.
The AY.4.2 data in this U.K. report are based on a relatively small sample size—about 13,000 people infected with AY.4.2, compared to over 350,000 people infected with the original Delta variant. Still, it’s good news that the variant appears to simply be more transmissible, not more able to break through vaccine-induced immunity or cause severe disease.
“More likely (I believe) is a slightly increased biological transmissibility,” Meaghan Kill wrote in a Twitter thread about this news. “Growth rate & secondary attack rates are refreshed with new data and findings remain the same as last week.” She predicts that AY.4.2 may be able to replace the original Delta by summer 2022.
How much is AY.4.2 spreading in the U.S.?
AY.4.2 has been identified in over 30 countries, including the U.S. But here, OG Delta continues to dominate; this variant has been causing over 99% of new cases in the U.S. for well over a month, with a couple of other Delta sub-lineages (AY.1 and AY.2) briefly popping up without getting competitive. AY.4.2 is not yet accounted for on the CDC’s variant tracker, but other estimates indicate that it’s causing under 1% of new cases in the U.S.
“We have on occasion identified the sublineage here in the United States, but not with recent increased frequency or clustering to date,” CDC Director Dr. Rochelle Walensky said at a recent COVID-19 briefing, according to STAT.
Are we prepared for a surge of AY.4.2—or another coronavirus variant?
The U.S. does not have a great track record for dealing with COVID-19 surges—whether that’s New York City in spring 2020 or Delta hotspots in the South this past summer. We’re doing more genomic sequencing than we were at the start of 2021, which helps with identifying potentially-concerning variants, but sequencing still tends to be clustered in particular areas with high research budgets (NYC, Seattle, etc.). And even when our sequencing system picks up signals of a new variant, we do not have a clear playbook—or easily-utilized resources—to act on the warning.
To illustrate this point, I’d like to share a major project of mine that was published this past week: an investigation of the Delta surge in Southwest Missouri this summer. This project was a collaboration between the Documenting COVID-19 project at the Brown Institute for Media Innovation and MuckRock (where I’ve been working part-time for a few weeks now), and the Missouri Independent, a nonprofit news outlet that covers Missouri state government, politics, and policy.
Missouri Independent reporter Tessa Weinberg and I went through hundreds of emails, internal reports, and other documents obtained through public records requests. We found that, even though Missouri had ample warnings about Delta—wastewater surveillance picked up the variant in May, and hospitals noticed increasing breakthrough cases in June—the Springfield area was completely overwhelmed by the virus. Infighting and mistrust between state and local officials also hindered the region’s response to the Delta surge.
Our major findings (copied from the article) include:
Springfield hospital and health department leaders urged the state to take advantage of additional genomic sequencing assistance to address unanswered questions about the variant’s spread. The state declined, forcing Springfield officials to seek additional data on their own.
After days of preparation for an overflow hospital for COVID patients requested by Springfield officials, local leaders decided to forego the plan after the window of need had passed — setting off dueling narratives over the reason why in public while state officials seethed in private.
When local officials pleaded for more support in addressing the Delta surge, state officials questioned the value of directing more resources to the area and even wondered whether the overflow hospital request was fueled by motivations to “pay for an expansion of their private hospital.”
You can read the full story here (at the Missouri Independent) or here (on MuckRock’s website). Find the documents that we used here.
And read my Twitter thread with more highlights here:
Leave a comment