This week, the CDC titled its weekly COVID-19 data report, “Keep Variants at Bay. Get Vaccinated Today.” I love a good rhyme, but the report also makes a valuable point: vaccinations not only protect individuals from coronavirus variants, they also reduce community transmission—slowing down future viral mutation.
Delta, or B.1.617.2, is particularly dangerous. As I’ve written before, this variant spreads much more quickly than other strains of the coronavirus and may cause more severe illness, though scientists are still investigating that second point. Thanks to this variant, it’s now much more dangerous to be unvaccinated than it was a year ago.
The Delta variant was first linked to a surge in India, but it’s now become dominant in the U.K., Russia, Indonesia, and other countries. As Eric Topol recently pointed out on Twitter, the variant’s dominance has led to sharp rises in cases—and in deaths—for these nations.
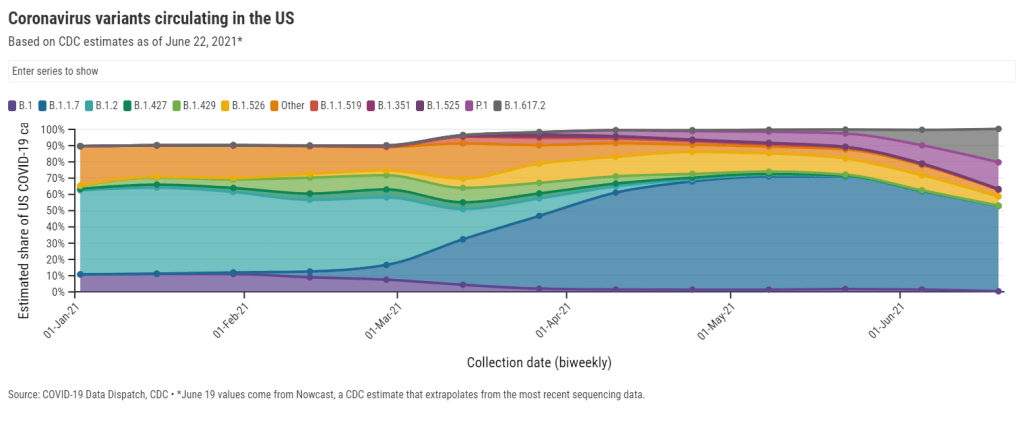
The U.S. is somewhat distinct from the U.K., though, because we had a more diverse group of variants circulating here before Delta hit. In the U.K., Delta arrived in a coronavirus pool that was 90% Alpha (B.1.1.7); here, the Alpha variant peaked at about 70%, with several other variants of concern also circulating.
In other words: we can’t forget about Gamma. Gamma, or P.1, was first identified in Brazil late in 2020. While it’s not quite as fast-spreading as Delta, it’s also highly transmissible and may be able to more easily re-infect those who have already recovered from a past coronavirus infection.
The Gamma variant now causes an estimated 16% of cases in the U.S. while the Delta variant causes 21%, per the CDC’s most recent data (as of June 19). Both are rapidly increasing as the Alpha variant declines, now causing an estimated 53% of cases.
A recent preprint from Helix researchers suggests an even starker change in the U.S.’s variant makeup. Helix’s analysis shows that Alpha dropped from 70% of cases in April 2020 to 42% of cases, within about six weeks.
Delta will certainly dominate the U.S. in a few weeks, but Gamma will likely be a top case-causer as well. Other variants that once worried me—like those that originated in New York and California—are getting solidly outcompeted.
The TL;DR here is, get vaccinated. Don’t wait. Tell everyone you know.
Leave a comment