RECOVER, the U.S.’s largest initiative to understand Long COVID, published a major scientific study this week in JAMA. The paper goes over key Long COVID symptoms and other findings from nearly 10,000 adults who have joined the project’s research cohort. Its authors propose a new, more specific definition for Long COVID, which will be used in future studies from this project.
This is a big milestone for RECOVER; it’s the first paper to actually share data from the study’s patient cohort, rather than from electronic health records. While the paper doesn’t provide any truly novel, previously unreported information about Long COVID, it confirms findings from smaller studies and validates patient experiences. It’ll certainly be valuable for thousands of scientists around the country struggling to understand this debilitating condition, though patients have expressed some concerns about the paper’s central framework.
This study is also a rather late milestone, considering that the National Institutes of Health received $1 billion in funding from Congress for this initiative in December 2020 (two and a half years ago), and started enrolling patients in fall 2021. For more details on RECOVER’s delays—and many criticisms it’s faced from patients and experts—please check out this investigation by me and Rachel Cohrs, at STAT News and MuckRock.
Here are a few key things you should know about the paper, and that you should watch out for while reading other articles about it:
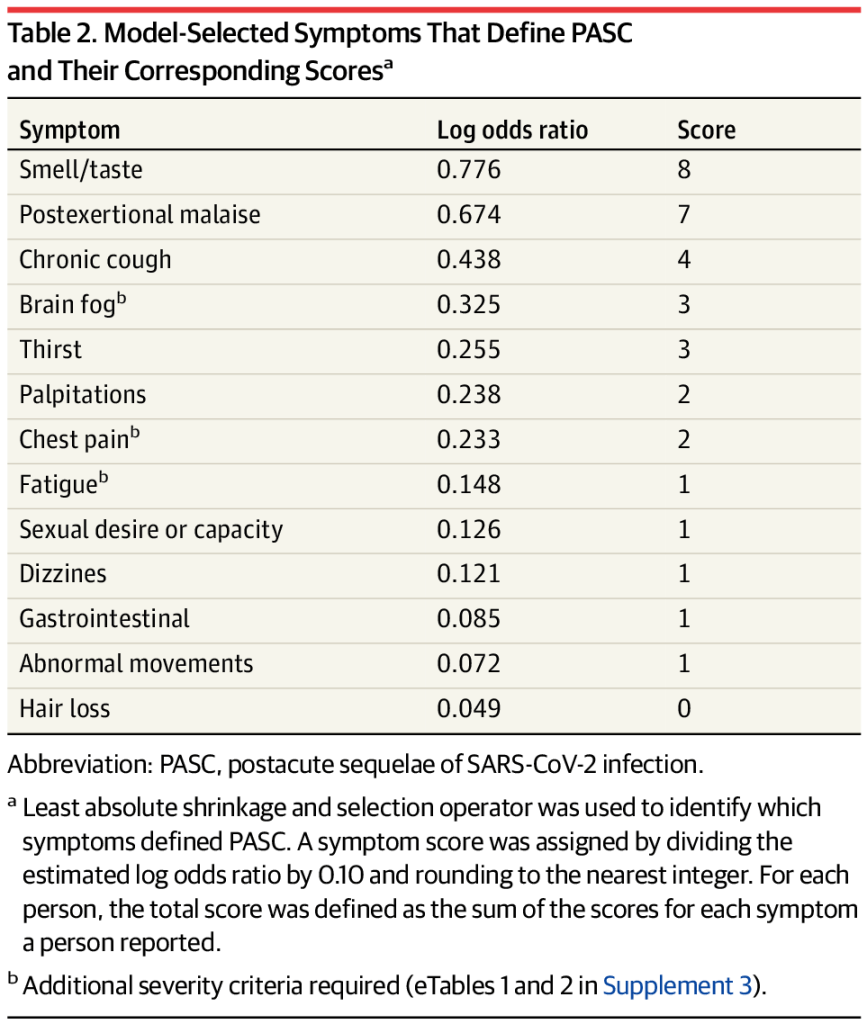
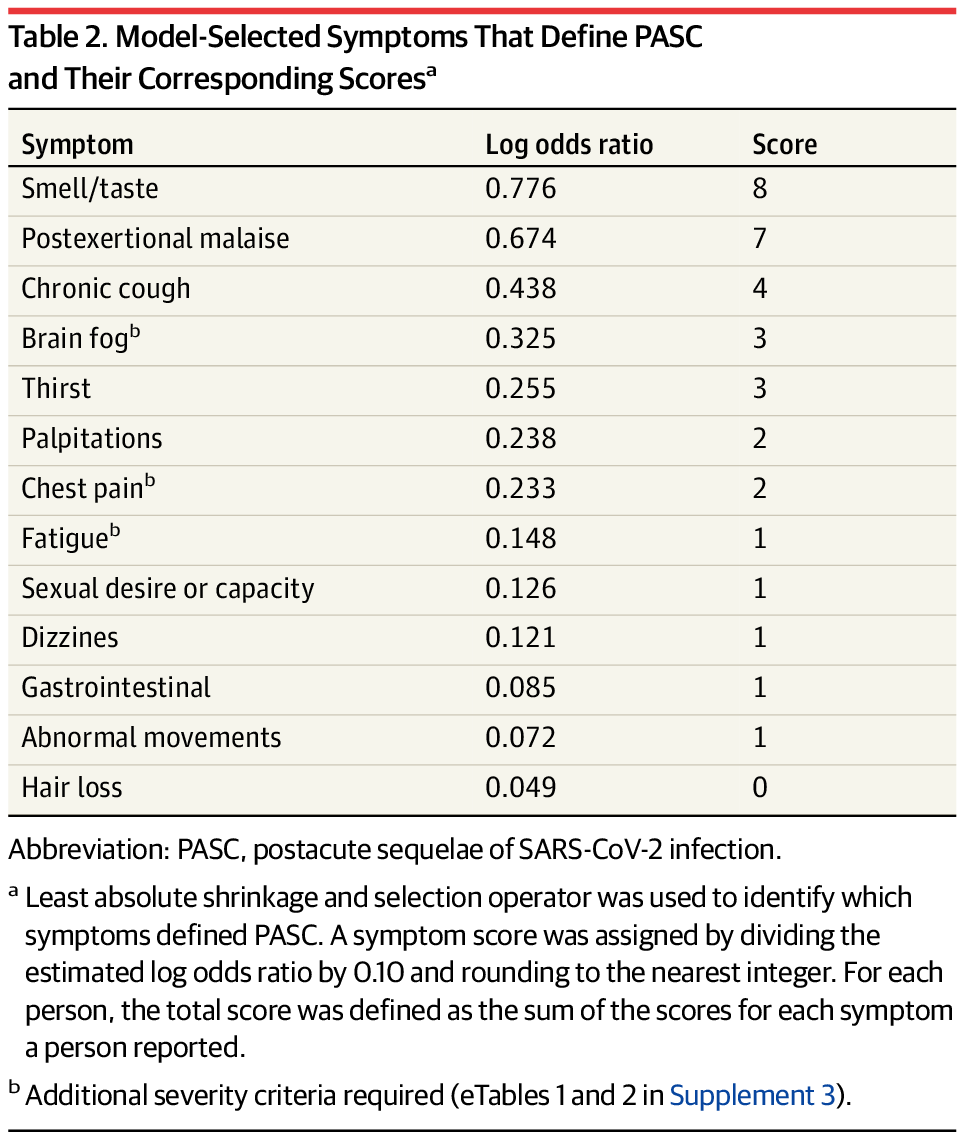
- The authors’ main goal was to determine which symptoms can specifically be used to diagnose long-term symptoms following a coronavirus infection. Using survey data from RECOVER’s participants, the researchers developed a framework that sorts patients into three categories: definitely having symptoms due to a past coronavirus infection (or “infected”), not having symptoms due to a past infection (“uninfected”), and possibly having symptoms due to a past infection (“unspecified”). This framework prioritizes symptoms unique to Long COVID, such as the loss of smell or taste, over those symptoms that are actually more debilitating for patients, such as chest pain or chronic fatigue. Also, as patient-expert Lisa McCorkell pointed out on Twitter, the unspecified category includes people with Long COVID.
- The paper highlights 12 Long COVID-specific symptoms; there are a lot more. I’ve seen some articles covering this study frame it as, “these are the 12 definitive symptoms of Long COVID.” That’s a misrepresentation of the results. In fact, the authors selected 12 common symptoms that are helpful for their framework (i.e. determining who had a coronavirus infection); we know from other research that Long COVID can include up to 200 different symptoms. RECOVER leader Leora Horwitz even acknowledged in a Twitter thread describing the paper that “these are not the ONLY symptoms that people have, nor are they necessarily the most important to patients, the most common, the most severe or most burdensome.”
- Long COVID is a spectrum, with different clusters of symptoms. This paper adds more evidence to support a hypothesis I’ve heard from many experts, that Long COVID is not one condition but a variety of overlapping conditions all caused by SARS-CoV-2. Different symptoms might be caused by different biological processes, and different patient groups could require different treatments. RECOVER has identified potential patient groups, which the researchers will study further (including through clinical trials, projected to start this summer).
- Long COVID has a wide variety of impacts on day-to-day life, but the most severe patients might not have the best proof. Using this paper’s framework, long-haulers can give themselves a “Long COVID score” reflecting how likely they are to have symptoms caused by a past coronavirus infection. But, as patient-expert Chris Maddison explained, a higher score doesn’t necessarily mean Long COVID has more drastically impacted the patient’s day-to-day life. “I would prefer to flip this, i.e., a def. that centers folks who are suffering regardless of whether we can accurately predict prior infection,” he wrote.
- Infection post-vaccination or with Omicron can lead to lower—but still significant—Long COVID risk, compared to earlier in the pandemic. Since RECOVER started recruiting in fall 2021, the study includes some people who were first infected during the first Omicron wave, then developed Long COVID symptoms afterward. About 10% of the patients infected during Omicron later developed symptoms, which pretty close to the study’s overall estimate of Long COVID prevalence (also about 10%). Vaccination or infection with an Omicron variant may make you less likely to get Long COVID, this study suggests, but the risk is still very present.
- Repeat infections may increase Long COVID risk. RECOVER was able to follow 2,150 people who got infected during the Omicron wave, including 81 who had multiple infections. Of those with multiple infections, 16 people—or one in five—had Long COVID symptoms within six months. That’s double the prevalence rate of those who just had one infection in the same timeframe (10%). While these are small numbers, the finding is certainly worth further study; see this thread from patient-expert Hannah Davis for more details.
- This is not a prevalence paper, and it does not provide a clinical definition of Long COVID. Some media coverage might suggest that this paper has “defined Long COVID,” which is a misrepresentation of the study. While the authors do propose a new framework for evaluating potential Long COVID patients, they make it clear that a lot more research and iteration will be needed before any RECOVER findings should be used in the doctor’s office. The paper also doesn’t provide a definitive answer on how many people get Long COVID, since it includes a relatively small number of people who were uninfected when they joined the study. Quoting Lisa McCorkell again: “It is very clear throughout the paper that in order for this to be actionable at all, iterative refinement is needed.”
- This won’t be the last paper sharing findings from the RECOVER cohort. This study presented data from patients’ symptom surveys, which is just one small part of the RECOVER cohort’s activities. The enrolled patients have also undergone extensive medical testing and symptom tracking over time, which will be the subject of future studies—and will be used to refine RECOVER’s Long COVID framework. Clinical trials will (eventually) provide more data as well.
To my fellow journalists covering this study: I highly encourage you to present this paper as a small part of a complicated, iterative research process, rather than a definitive answer to long-standing questions about Long COVID. I also encourage you to talk to patient-experts and ask for their criticisms of the study (like those I’ve cited here), rather than just letting the RECOVER leadership go unchallenged.
Leave a comment