Remember when I said “we’ll see if anything else happens” in last week’s article on AstraZeneca’s issues? Well, I accept full responsibility for manifesting the chaos that happened earlier this week and I promise I won’t tempt fate again this time around. If you’re confused, as I certainly was, here’s just what the hell happened.
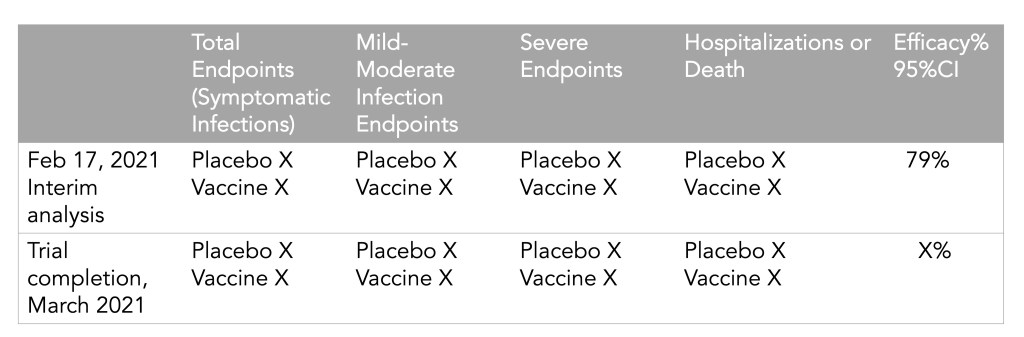
On Monday, AstraZeneca released results from their Phase 3 trials in the United States, and they looked good: 79% efficacy against symptomatic disease, 100% efficacy against hospitalizations and deaths. This was certainly a welcome result for the company which is continuing to grapple with fallout from rare cases of blood clots that have been reported in some people after they got the vaccine, and gears started to turn to get EUA approval in the United States. (Even though, again, the U.S. just promised most of their supply to Canada and Mexico. Everyone wants FDA clout, I guess.)
But on Tuesday, officials started to question the results. The results released on Monday had looked better than more recent results released elsewhere, one of which showed an overall efficacy of around 60%. Also, as Dr. Eric Topol pointed out, the data were fairly incomplete:
Independent reviewers from the data and safety monitoring board sent “a harsh note” to AstraZeneca, according to Anthony Fauci, and sure enough, it soon became clear that AstraZeneca had released outdated (better) numbers instead of the real results from the trial, obfuscating how efficacious the vaccine actually was in the U.S. trial.
After all this, on Wednesday morning, AstraZeneca released the updated overall efficacy number: 76%. All that drama over docking three percentage points. (Though they did also complete the dataset, thus satisfying Dr. Topol and saving them more of his very pointed tweets. Thank you Dr. Topol.)
Dr. Ashish Jha sums it up pretty well:
But Roxanne Khamsi sums it up even better:
We’ll see if anything el—nope, I promised I wouldn’t.
Related posts
- Sources and updates, November 12Sources and updates for the week of November 12 include new vaccination data, a rapid test receiving FDA approval, treatment guidelines, and more.
- How is the CDC tracking the latest round of COVID-19 vaccines?Following the end of the federal public health emergency in May, the CDC has lost its authority to collect vaccination data from all state and local health agencies that keep immunization records. As a result, the CDC is no longer providing comprehensive vaccination numbers on its COVID-19 dashboards. But we still have some information about this year’s vaccination campaign, thanks to continued CDC efforts as well as reporting by other health agencies and research organizations.
- Sources and updates, October 8Sources and updates for the week of October 8 include new papers about booster shot uptake, at-home tests, and Long COVID symptoms.
- COVID source shout-out: Novavax’s booster is now availableThis week, the FDA authorized Novavax’s updated COVID-19 vaccine. Here’s why some people are excited to get Novavax’s vaccine this fall, as opposed to Pfizer’s or Moderna’s.
Leave a comment